Tooth pain, sensitivity, or visible damage are often clear signs that you may need a root canal or a dental crown. In general, a root canal is required when the inner pulp of the tooth becomes infected or inflamed, causing persistent pain, swelling, or sensitivity.
If you’re experiencing symptoms like lingering sensitivity to hot or cold, severe toothache, discoloration, or pain when chewing, it may indicate deeper damage that requires professional care in Mesa, AZ. In many cases, both treatments are used together with a root canal to remove infection and a crown to restore strength.
Do You Need a Root Canal or a Crown?
Understanding the signs of root canal or crown treatment can help you identify problems early and get timely dental care to protect your smile in Mesa, AZ.
Signs You May Need a Root Canal
- Persistent, throbbing tooth pain that doesn’t go away on its own
- Sensitivity to heat or cold that lingers well after the source is removed
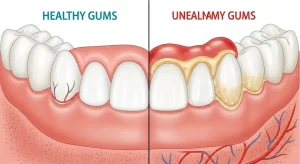
- Swollen, tender, or discolored gums near one specific tooth
- A pimple-like bump on the gum near the affected tooth
- Tooth discoloration particularly a grey or darkening tone
- Pain when biting down or applying any pressure to the tooth
Signs You May Need a Dental Crown
- A visibly cracked, chipped, or fractured tooth
- A large filling that is failing or covers most of the tooth’s surface
- A tooth that has become structurally weak after previous dental treatment
- Significant wear from grinding or acid erosion
- Severe cosmetic damage affecting the tooth’s shape or appearance
When You Might Need Both
When the inner pulp of a tooth is infected and a root canal is performed, the tooth is left hollowed out and significantly weakened. In most cases especially for back teeth a crown is placed afterward to protect remaining structure and restore full function. A root canal without a follow-up crown on a molar is one of the most common causes of tooth fracture after treatment.
What Is a Root Canal and When Is It Needed?
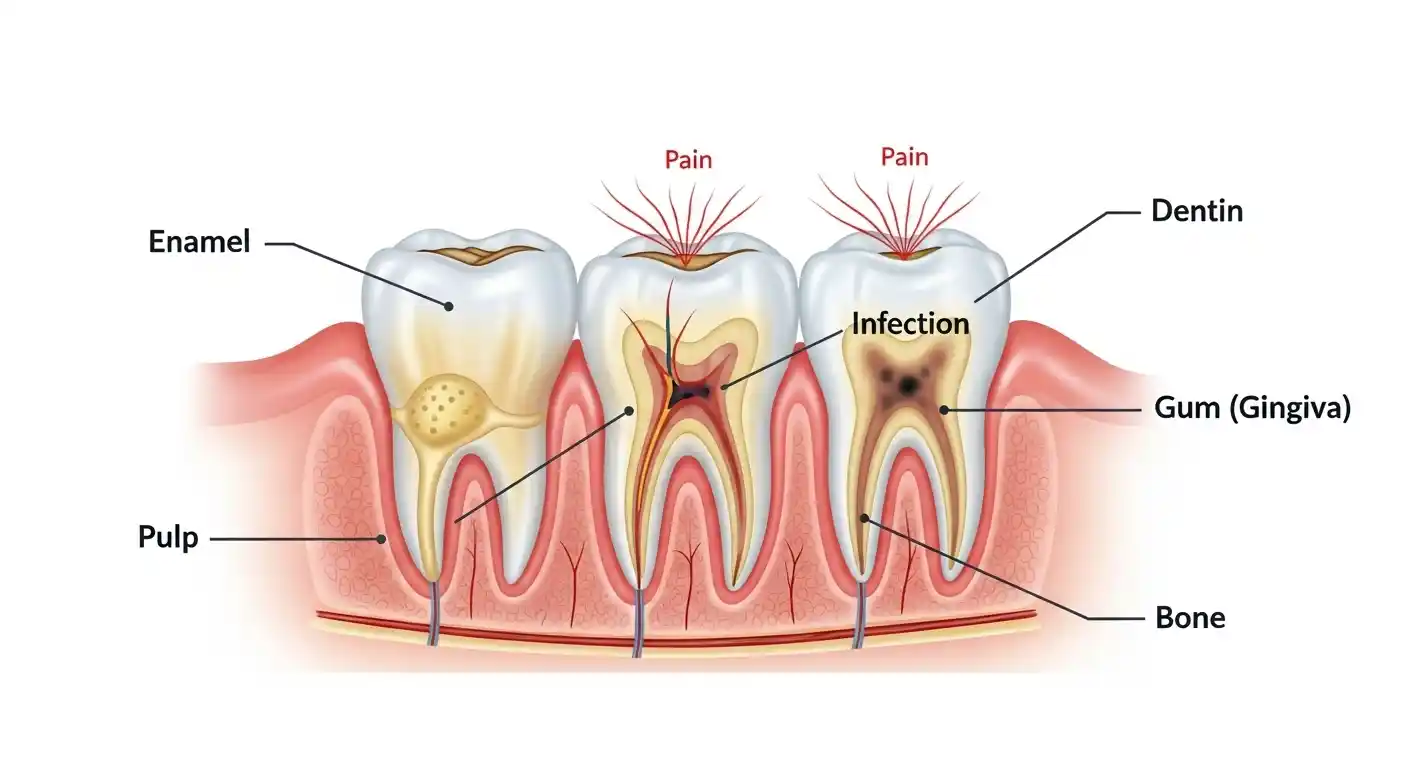
A root canal is a dental procedure used to remove infected, inflamed, or dead tissue from inside a tooth. Each tooth contains a soft inner layer called the pulp, which includes nerves and blood vessels that keep the tooth alive.
When bacteria enter the tooth through deep decay, a crack, or repeated dental procedures, the pulp can become infected and painful. If left untreated, this infection can spread to the surrounding bone and tissues, leading to more serious oral health complications.
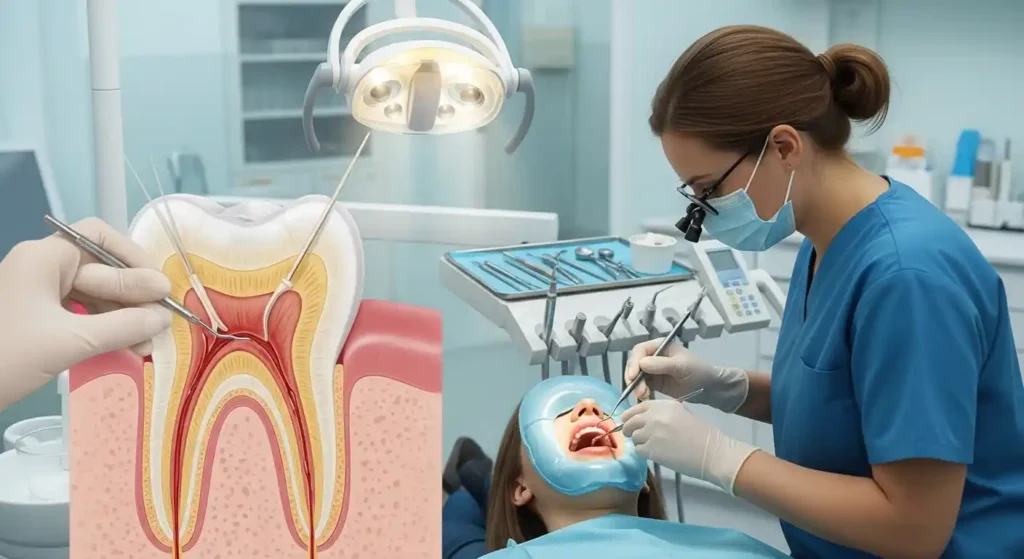
What Happens During a Root Canal Procedure
During the procedure, the dentist or endodontist numbs the area with a local anesthetic and creates a small opening in the tooth. The infected pulp is carefully removed, and the inner canals are cleaned, shaped, and disinfected. The space is then filled with a rubber-like material called gutta-percha and sealed to prevent reinfection. In most cases, a dental crown is placed later to protect and strengthen the treated tooth.
Despite its reputation, a root canal is typically no more uncomfortable than getting a filling. Most patients feel pressure rather than pain, as the area is fully numbed during treatment.
Common Signs You May Need a Root Canal
Persistent tooth pain is the most telling indicator. Unlike a passing toothache, the pain from an infected pulp tends to be deep, throbbing, and constant, often radiating to the jaw, ear, or temple.
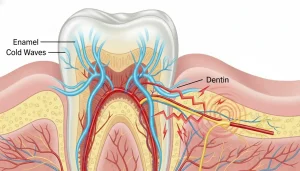
Lingering sensitivity to hot or cold is another key sign. Brief temperature sensitivity is normal in most teeth. When that sensitivity persists for 10 seconds or more after the source is removed, it often signals pulp inflammation or damage.
Swollen or tender gums near one specific tooth particularly when localized and slow to resolve suggest infection spreading from the pulp into surrounding tissue.
Tooth discoloration, especially a greyish or brownish tone, indicates the internal blood supply has been compromised. A dying or dead tooth often changes color as the pulp breaks down internally.
Pain when biting or chewing that worsens rather than resolves is a warning sign that internal inflammation is placing pressure on the ligament surrounding the tooth root.
A pimple on the gums known as a dental sinus tract or fistula is one of the clearest visible signs of an abscess. This small raised bump near an affected tooth may release fluid and often appears and disappears repeatedly until the underlying infection is treated.
What Is a Dental Crown and When Is It Recommended?
A dental crown is a custom-fitted cap that covers the entire visible portion of a tooth from the gumline up. It restores the tooth’s shape, size, strength, and appearance and with proper care, can last 10 to 15 years or more.
What Does a Dental Crown Do?
Crowns serve both protective and restorative purposes. They hold a cracked tooth together, reinforce a tooth weakened by large decay or previous dental work, replace a failing large filling, restore a tooth worn down by grinding, and improve the appearance of severely damaged or discolored teeth. They are also used to anchor dental bridges and cap dental implants.
Signs You May Need a Dental Crown
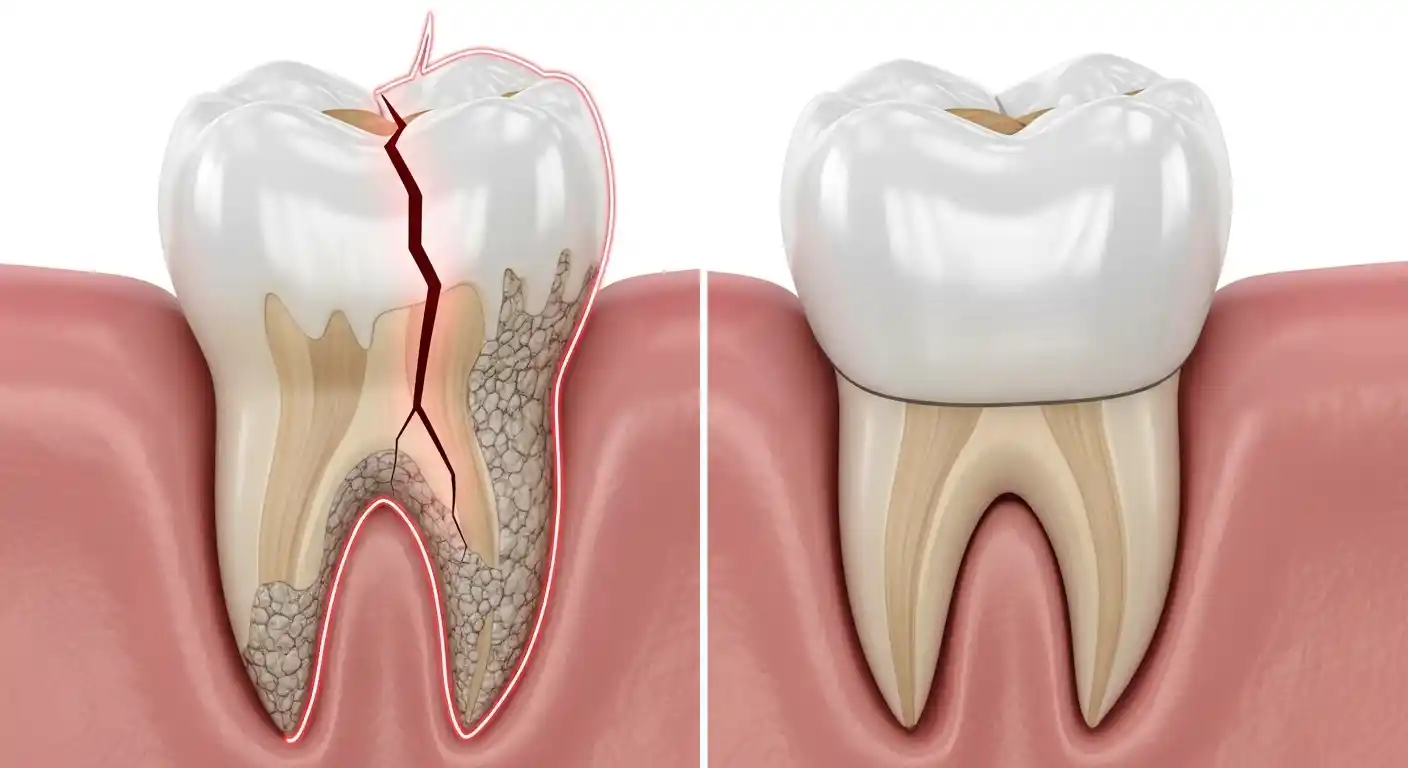
A cracked or chipped tooth is one of the most common reasons crowns are placed. A minor chip may be repaired with bonding, but when a crack runs deeper particularly when it causes pain on biting a crown is typically necessary to hold the tooth together and stop the crack from propagating further.
A large or failing filling that covers more than half the tooth’s surface compromises the remaining natural structure significantly. A crown provides full coverage and a far more durable long-term result than a large filling alone.
Worn-down teeth from bruxism or acid erosion lose height and strength over time to the point where crowns are needed to rebuild bite function and protect remaining structure.
A weakened tooth after treatment, particularly after a root canal, where the interior has been hollowed out needs a crown to prevent fracture under normal chewing forces.
Significant cosmetic damage that affects appearance can also warrant a crown, though veneers or bonding may be more appropriate when the tooth is structurally sound and only aesthetics are the concern.
Early vs Advanced Signs of Tooth Damage
Understanding the difference between early and advanced symptoms can help you seek treatment at the right time and prevent more serious dental problems.
Early Warning Signs
Early-stage problems are often subtle which is exactly what makes them easy to dismiss. Mild temperature sensitivity that resolves quickly, a small visible crack that causes no pain, occasional discomfort when biting specific foods, and minor gum tenderness near one tooth are all worth mentioning at your next dental visit.
At this stage, treatment is straightforward and minimally invasive. A filling, bonding, or a crown may be all that is needed. The damage has not yet reached the pulp, and a root canal is unlikely to be necessary.
Advanced Warning Signs
When early signs are ignored, conditions worsen. Severe spontaneous pain, especially pain that wakes you at night signals pulp involvement. Visible swelling in the gum, jaw, or face means infection has spread beyond the tooth itself. A tooth that feels loose, or decay so extensive that most of the visible tooth is destroyed, indicates serious structural and possibly bone damage. At this stage a root canal is almost unavoidable, and extraction becomes a real possibility if treatment is delayed any further.
Root Canal vs Crown: What’s the Difference?
Understanding the difference between a root canal and a dental crown can help you make informed decisions about your oral health and choose the right treatment at the right time.
Key Differences Explained Simply
A root canal treats the inside of the tooth by removing infected or damaged pulp to relieve pain and stop infection. A dental crown, on the other hand, covers the outside of the tooth to restore its strength, shape, and function. In simple terms, a root canal fixes internal problems, while a crown protects the outer structure.
Can You Need Both a Root Canal and a Crown?
Yes, in many cases both treatments are needed. A root canal removes the infection but can leave the tooth weaker, which is why a crown is often placed afterward to protect it and restore strength.
For back teeth like molars, a crown is usually recommended after a root canal due to the pressure from chewing, while in some front teeth cases, a crown may not always be necessary if enough healthy tooth structure remains.
Can a Crown Be Done Instead of a Root Canal?
When a crown alone is enough: If the tooth is damaged or weakened but the pulp is still healthy and free from infection, a crown resolves the problem without the need for a root canal. A cracked tooth with no pulp involvement, or a tooth with a large failing filling and a structurally sound pulp, typically needs only a crown.
When a root canal is necessary: If the pulp is infected, inflamed, or dead, no external restoration will resolve the underlying problem. Placing a crown over an infected tooth without treating the pulp first traps the infection, which continues to spread through the root and into surrounding bone. A root canal must come first.
Risks of the wrong treatment: Skipping a necessary root canal in favor of a crown alone leads to worsening infection, abscess formation, bone loss, and ultimately tooth loss. This is why accurate professional diagnosis, not self-diagnosis, is essential before any treatment decision is made.
How Dentists Decide Which Treatment You Need
Dentists use exams, symptoms, and diagnostic tools to determine whether a root canal or dental crown is needed. The goal is to accurately assess the tooth and choose the most appropriate treatment while preserving as much natural tooth structure as possible.
Diagnostic Factors
Dentists evaluate the severity of tooth decay through a visual exam and gentle probing to see how deep the damage goes. They also assess whether the tooth pulp is involved by reviewing your symptoms, pain patterns, and test results.
X-rays are used to check the condition of the tooth roots, surrounding bone, and to detect any hidden infection or abscess. In addition, your pain level and symptom history such as lingering sensitivity, spontaneous pain, or swelling provide important clues to help guide the diagnosis.
How Dentists Diagnose the Problem (X-Rays and Exams)
A complete diagnosis involves several steps. A visual examination helps identify visible issues such as cracks, decay, discoloration, and gum changes. Digital X-rays allow dentists to see beneath the surface, including the root structure, bone levels, and hidden signs of infection.
Sensitivity and pulp tests, such as cold tests or electric pulp testing, are used to determine whether the tooth’s nerve is healthy, inflamed, or no longer alive. Together, these tools give your dentist a clear and accurate picture of your tooth’s condition, ensuring the right treatment is recommended without unnecessary procedures.
How Long Does Each Treatment Take and Recovery Time
Understanding the timeline and recovery process for each treatment can help you know what to expect and plan your care with confidence.
Root Canal Timeline and Recovery
A root canal on a front tooth can often be completed in a single appointment lasting about 60 to 90 minutes. However, molars with multiple canals may require two visits to fully treat the tooth.
After the procedure, it is normal to experience mild soreness or tenderness for two to three days, which can usually be managed with over-the-counter pain relievers. Full recovery typically takes about one to two weeks. In most cases, a dental crown is recommended soon after to protect and strengthen the treated tooth.
Crown Procedure Timeline and Recovery
A traditional crown requires two appointments, one for tooth preparation and impressions, and a second one to two weeks later for permanent crown placement. Same-day CEREC crowns can be completed in a single visit of one to two hours. After placement, mild sensitivity at the gumline is common for a few days and resolves on its own in the majority of cases. There is no significant downtime associated with crown placement.
What Happens If You Delay Treatment?
Delaying treatment for a dental issue can allow the problem to worsen over time. A small cavity or mild pain can develop into a deeper infection, leading to severe tooth pain, swelling, and possible damage to the surrounding teeth and gums.
If left untreated, the infection can spread to the tooth’s root and nearby bone, increasing the risk of needing more complex and costly procedures like a root canal or even tooth extraction. Acting early helps preserve your natural tooth and prevents more serious complications.
Can You Prevent Needing a Root Canal or Crown?
You can reduce your chances of needing a root canal or dental crown by maintaining good oral hygiene and visiting your dentist regularly. Brushing twice a day, flossing daily, and using fluoride toothpaste help prevent decay and gum disease, which are common causes of serious tooth damage.
Regular dental checkups allow your dentist to detect problems early before they become severe. Avoiding habits like teeth grinding, chewing hard objects, and consuming too much sugar can also help protect your teeth and keep them strong over time.
When Should You See a Dentist Immediately?
You should see a dentist immediately if you experience severe tooth pain that does not go away, swelling in your gums, jaw, or face, or signs of infection such as a pimple-like bump on the gums. These symptoms may indicate a serious issue like an abscess or deep infection that requires prompt treatment to prevent it from spreading.
You should also seek urgent care if you have a broken, cracked, or knocked-out tooth, or if you notice sudden sensitivity, bleeding, or a tooth becoming loose. Acting quickly can help save your tooth and avoid more complex procedures in the future.
Expert Dental Care You Can Trust in Mesa, AZ
If you’re experiencing tooth pain, sensitivity, or visible damage, don’t wait, early treatment can make all the difference. Schedule a consultation with our experienced dental team at Valencia Dental Care in Mesa, AZ today. We’ll evaluate your symptoms, recommend the right treatment, and help you protect your smile with personalized care you can trust.
Conclusion
Understanding the signs that indicate you may need a root canal or a dental crown is essential for protecting your oral health. Early diagnosis and treatment can relieve pain, stop infection, and help preserve your natural teeth. If you notice any symptoms such as persistent pain, sensitivity, or visible damage, don’t delay prompt dental care can prevent more serious complications and help you maintain a healthy, confident smile.
Frequently Asked Questions
How do I know if I need a root canal or a crown?
A root canal is needed when the inner pulp of the tooth is infected or damaged, causing pain or swelling. A crown is recommended when the tooth is weak, cracked, or damaged but the pulp is still healthy.
Is a root canal painful?
Modern root canal treatments are typically no more painful than getting a filling. The procedure is done under local anesthesia, so you should not feel pain during treatment.
How long does a dental crown last?
With proper care, dental crowns can last 10 to 15 years or even longer. Good oral hygiene and regular dental visits can extend their lifespan.
Can a crown fix a cracked tooth?
Yes, a crown can hold a cracked tooth together and prevent the crack from worsening. It also restores strength and function to the damaged tooth.
What happens if I delay treatment?
Delaying treatment can allow infection or damage to worsen, leading to severe pain, abscess formation, and possibly tooth loss. Early treatment helps avoid more complex and costly procedures.